From Extreme Prematurity to Remarkable Progress: Alexander's Story
How Parent and Family Education Provided Lifesaving Skills to the Parents of a Premature Baby With a Severely Compromised Airway
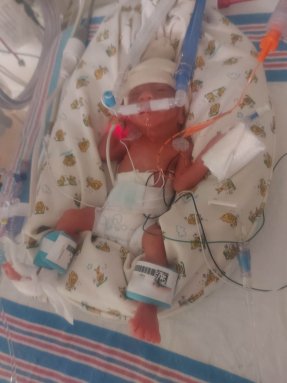
Born at just 24 weeks, Alexander faced extraordinary, life-threatening challenges from his first moments. He required resuscitation at birth and was placed on CPAP, a form of breathing support, in the delivery room. In the NICU, he was diagnosed with chronic lung disease (bronchopulmonary dysplasia) and severe subglottic stenosis, a dangerous narrowing of the airway just below the vocal cords. He required a tracheostomy (a breathing tube in his neck), ongoing ventilator support, and a gastrostomy tube for feeding.
In July 2025, at 7 months old, Alexander was admitted to Blythedale Children’s Hospital for ventilator weaning and comprehensive rehabilitation. He arrived requiring 28% supplemental oxygen through CPAP.
“In the pediatric airway, even a small amount of swelling can significantly impact breathing,” said Dr. Shahrzad Mohammadi. “When he first came to us, he was breathing very fast and was using excessive respiratory muscles in order to breathe, tiring quickly.”
Blythedale’s multidisciplinary team collaborated closely with specialists at Maimonides Medical Center — where he was born — to better understand the cause of Alexander’s airway swelling. Once it was determined that acid reflux was contributing to his condition, the team implemented targeted medication management and feeding strategies to reduce irritation and protect his airway.
At the same time, Alexander’s parents, Paola and Vianni, began training through Blythedale’s Parent and Family Education program to prepare for his care at home.
“At first, I was a little nervous because we didn’t know what to expect,” said Vianni.
The program breaks down complex care into manageable steps, teaching families how to care for a child’s tracheostomy, ventilator, medications and gastrostomy tube. Because of Alexander’s narrowed airway, his parents also received specialized training to respond in emergencies.
“For children with critical airways like Alexander’s, parents are taught how to advocate for their child with emergency personnel,” said Angela Brennan Larkin, MSN, Ed, RN, director of the Parent and Family Education program.
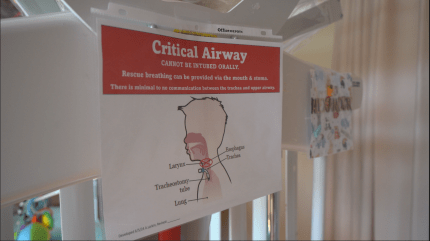
In an emergency, Alexander cannot be intubated. If his tracheostomy becomes dislodged, it is critical that his stoma, the opening in his airway, remains open. Larkin developed a customized curriculum that the family can share with first responders to ensure they understand how to provide lifesaving care specific to Alexander’s needs.
“When families are at home, they are the experts,” Larkin said. “We want them to feel confident and competent in providing lifesaving care.”
During his time at Blythedale, Alexander made steady progress. He was gradually weaned off CPAP and now uses a tracheostomy collar for up to 12 hours a day, breathing independently and requiring ventilator support only at night. His care team is hopeful that, with continued progress, he may eventually be able to have his tracheostomy removed.

“The therapies at Blythedale have not just been great — they’ve been fantastic,” Paola said. “When we arrived, he was unable to move. Today, he’s standing on his own.”
Through intensive speech, feeding, occupational, and physical therapies, Alexander has begun reaching key developmental milestones. He is learning to stand independently and has started to crawl. During a recent music therapy session, he actively engaged with instruments, responding to rhythm and sound — a meaningful sign of his continued growth and development.
Next month, Alexander will return home to be with his family and his older sister; a milestone they have long awaited.




